
I have been wondering lately if it’s just my imagination or if Lyme research and awareness are finally getting traction. Because funding has been pretty dismal historically. But the situation is improving bit by tiny bit.
Staying grounded while recovering from Lyme disease

Don’t be put off by the science lingo—click on the image to download and play a Powerpoint of the nanotrap at work. Cool, right?
Courtesy of Dr. Lance Liotta, George Mason University.
Several years ago after gardening in my suburban backyard, I found a deer tick attached to my hip. Then came a rash. And then I started hurting all over like I was getting the flu.
I wasn’t surprised when my nurse practitioner examined me, diagnosed Lyme, and prescribed antibiotics. I should have been lucky. I had the bite with the beast still attached, in the middle of the classic target rash. I felt like I was dying of flu-like aches and pains.
But as it turned out, I wasn’t lucky after all. Continue reading

I’m always a little stunned when I track this blog and am reminded that people from all over the world visit. So many of us are on the lookout for information.
Today I’m thinking about Canadians because lots of my traffic at the moment is coming from my neighbors to the north, who’ve been checking out my post from several years ago on how Lyme was affecting my brain at the time. Looks like some of you are sharing the link on Facebook. Thank you!
Like others around the globe, many Canadians are having a tough time getting good treatment. Health officials just don’t get it (sound familiar?).
The nonprofit Canadian Lyme Disease Foundation says: Continue reading
If you’re like me, you want to know the latest scoop on what scientists are learning about Lyme disease. In this May 2013 interview we hear again from pathologist Alan MacDonald. (This interview is part 2 of a 3-part series, see the first one here). I’ve noted some key points you can jump to if you don’t have time to view the entire interview.
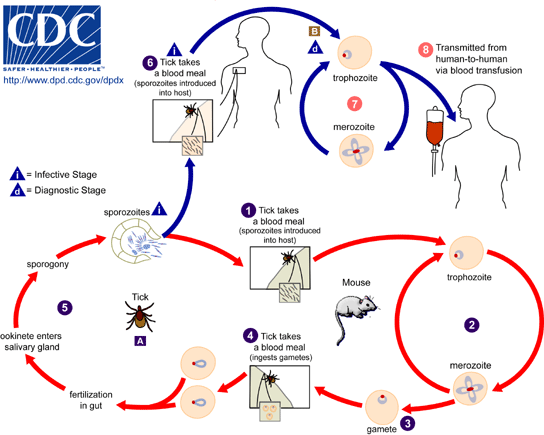
Babesia Life Cycle.
From the U.S. Centers for Disease Control (CDC).
When I finally arrived at the door of a Lyme Literate Doctor (LLMD), I was surprised to learn that in addition to Lyme, I have an infection of the red blood cells called Babesiosis, caused by a tiny parasite.
Symptoms can include fatigue, drenching sweats, muscle aches, and nausea; the infection often begins with a high fever. It can also attack the spleen. I got mine from a tick bite. People also become infected through blood transfusions.
Did you hear whoops of excitement from Virginia this week?
A history-making bill (SB971) that would require doctors to inform patients of the inaccuracy of Lyme testing is under consideration right now in my great state. I would have traveled to Richmond to support the bill in person, if I weren’t so ill with lyme myself.
Above is a video from YouTube of the January 29 debate in the state Senate earlier this week. If you are aren’t a hearing junkie, scan for the opposition’s argument, and fast-forward to these sections for compelling highlights:
[15:15] Senator Richard H. Black, who introduced this bill. When asked if consideration has been made as to how the bill could intrude on patient/physician relationships (many doctors oppose the bill), Senator Black replies respectfully, “I have tremendous faith in our physicians and I believe in their ability to do their jobs. I feel like in this particular area [Lyme disease] that this is a measure that would be of assistance and I think that it is something we owe to the people in the vast areas of Virginia that are afflicted by this.”
The Senator then cites incidence charts [21:15] and says that while his district is ground zero for Lyme in Virginia, other areas also have a very high incidence.
 Everyone, everywhere should read these tips from experts at the International Lyme and Associated Diseases Society (ILADS), reproduced here from the ILADS website with permission.
Everyone, everywhere should read these tips from experts at the International Lyme and Associated Diseases Society (ILADS), reproduced here from the ILADS website with permission.
Chronic Lyme disease patients may face a long hard fight to wellness. People with chronic Lyme can have many debilitating symptoms, including severe fatigue, anxiety, headaches, and joint pain. Without proper treatment, chronic Lyme patients have a poorer quality of life than patients with diabetes or a heart condition.
The fact is Lyme is a complex disease that can be highly difficult to diagnose. Reliable diagnostic tests are not yet available which leaves many—patients and physicians alike—relying on the so called “telltale signs” of Lyme disease: discovery of a tick on the skin, a bull’s eye rash, and possibly joint pain. However, ILADS research indicates that only 50%-60% of patients recall a tick bite; the rash is reported in only 35% to 60% of patients; and joint swelling typically occurs in only 20% to 30% of patients. Given the prevalent use of over the counter anti-inflammatory medications such as Ibuprofen, joint inflammation is often masked.

Taking care of yourself isn’t, well, rocket science…
[Dr. Robert Goddard. Credit: NASA on Flickr/The Commons]
Here are some lessons I’ve learned. Maybe you can benefit by taking them to heart now, instead of learning the hard way like I did over time and missing out on benefits you could have enjoyed much, much sooner. Continue reading